Rapid, evidence-based care saves lives. Use this guide to recognize what the most common treatment for 8 diseases in dogs looks like at the vet, what you can do at home, and how to prevent repeat episodes. This is education—not a substitute for your veterinarian.
At-a-Glance: What Treatment Usually Looks Like
| Condition | Most common veterinary treatment | What you do at home | Prevention |
|---|---|---|---|
| Parvovirus | Hospitalization, IV fluids/electrolytes, anti-nausea, antibiotics for secondary infection, early nutrition | Rest, finish meds, strict hygiene | Core vaccination on schedule |
| Kennel cough (CIRDC) | Mostly supportive care; antitussives; antibiotics only if complicated | Humidify air, harness (not collar), avoid excitement | Bordetella/CPiV/CAV-2 vaccines + reduce exposure |
| Leptospirosis | Doxycycline (± initial penicillin), IV fluids; dialysis if severe | Hygiene (zoonotic), complete meds | Vaccinate where risk exists |
| Heartworm disease | Doxycycline + preventive, then melarsomine 3-dose, strict exercise restriction | Leash walks only; monitor for cough/lethargy | Year-round preventives |
| Atopic dermatitis | Rapid itch control (oclacitinib/lokivetmab ± short steroids), topicals, ± cyclosporine; consider immunotherapy | Medicated baths/wipes, flea control | Trigger management, ASIT |
| Osteoarthritis | NSAIDs first-line, weight control, rehab/omega-3; add adjuncts as needed | Controlled, low-impact exercise, ramps/rugs | Keep lean; early OA plans |
| Otitis externa | Cytology-guided combo ear drops (antibiotic + antifungal + steroid); cleaning; treat the cause | Proper cleaning; rechecks | Address allergies/anatomy |
| Diabetes mellitus | Insulin, diet consistency, glucose monitoring; regular rechecks | Give insulin on schedule; keep logs | Weight control; screen at-risk breeds |
1) Parvovirus (Parvo): Supportive Care Saves Lives

What it looks like & how vets confirm it
Parvo strikes fast: vomiting, profuse/bloody diarrhea, dehydration, lethargy, fever or low temperature—most common in under-vaccinated pups. Diagnosis is by fecal antigen tests and/or PCR, interpreted with the history and exam. Because the virus shreds the gut lining and triggers sepsis risk, time to treatment is everything.
The most common treatment (hospital-first)
For the Most Common Treatment For 8 Diseases In Dogs, parvo is the clearest example of hospital-level supportive care as the lifesaver:
- IV fluids + electrolytes to reverse dehydration and shock.
- Antiemetics to control vomiting and enable nutrition.
- Broad-spectrum antibiotics to counter bacterial translocation from the damaged gut.
- Early enteral nutrition as soon as vomiting is controlled—feeding the gut improves outcomes.
- Pain control, glucose monitoring, and careful nursing in isolation.
This protocol is the evidence-based standard and dramatically improves survival compared with home-only care.
New adjunct many clinics now use: CPMA (monoclonal antibody)
Since 2023, a USDA-conditionally approved monoclonal antibody (Elanco’s CPMA) has been available as a single IV dose to neutralize parvovirus; in 2025 its label expanded to allow passive-immunity (prophylactic) use after exposure. Clinics use CPMA in addition to core supportive care to reduce viral load and ease case management. Ask your vet if CPMA is appropriate and available in your area.
Home care after discharge (how you help recovery)
- Strict rest; no dog parks or daycare.
- Give every medication exactly as directed (antiemetic, GI protectants, antibiotics if prescribed).
- Small, frequent meals of the vet-recommended diet; track water intake, appetite, stool, and energy daily.
- Isolate from other dogs until your vet clears you—parvo is wildly contagious.
Disinfection & isolation (stop the spread)
Parvo can persist in the environment for months. Clean visible mess first, then disinfect:
- Bleach (5–6% sodium hypochlorite) at 1:32 (½ cup per gallon of water) on clean, non-porous surfaces; respect contact time, then rinse.
- Accelerated hydrogen peroxide or potassium peroxymonosulfate products are effective alternatives where bleach isn’t suitable (follow label).
- Wash hands, launder bedding hot, and keep pups separate from contaminated areas.
Prevention that works (vaccine timing matters)
Parvo is a core vaccine. Because maternal antibodies can block early doses, pups are revaccinated every 2–4 weeks until >16 weeks old (many experts prefer 18–20 weeks in high-risk areas), then boosted per guideline. Adults get regular boosters based on risk and product label. Your vet will follow AAHA/WSAVA schedules for your region.
Red flags & what not to do
Go to the ER now for persistent vomiting, bloody diarrhea, weakness/collapse, sunken eyes, cold extremities, or black tarry stools. Do not try to manage parvo at home with oral fluids alone—hospital therapy is the survival driver, with or without CPMA.
Bottom line: For parvo, the most common treatment is aggressive in-hospital supportive care (fluids, antiemetics, antibiotics, early nutrition) in strict isolation; CPMA is a newer adjunct some clinics add. Pair that with thorough disinfection and proper vaccination timing to protect your next puppy and your community.
2) Kennel Cough / CIRDC: Mostly Supportive—Target Antibiotics Only When Needed

What it looks like & how vets confirm it
Kennel cough—now usually called CIRDC (canine infectious respiratory disease complex)—presents as a dry, hacking, “goose-honking” cough, often with gagging or small amounts of foam, a normal appetite, and no fever in uncomplicated cases. It’s a syndrome, not a single germ; common players include Bordetella bronchiseptica, canine parainfluenza virus, adenovirus-2, mycoplasma, and sometimes canine influenza. Your vet rules out pneumonia and tracheal issues with a focused exam, history (daycare/boarding/dog-park exposure), and—when indicated—thoracic radiographs, CBC/chemistry, or PCR panels.
The most common treatment (uncomplicated cases)
For this condition, the Most Common Treatment For 8 Diseases In Dogs playbook is primarily supportive care:
- Rest & reduce excitement (cough spikes with activity).
- Harness, not a neck collar (less tracheal irritation).
- Humidification (cool-mist humidifier or steamy bathroom sessions) to soothe airways.
- Targeted antitussives prescribed by your vet (e.g., hydrocodone or butorphanol) only when the cough is non-productive and keeping the dog from sleeping.
- Anti-inflammatories may be used if there’s significant airway irritation—only under veterinary guidance.
- No OTC human cough/cold meds unless your veterinarian explicitly okays a specific product and dose.
Most uncomplicated cases improve within 7–10 days and resolve by 2–3 weeks with rest and symptom control alone.
When antibiotics or escalated care are appropriate
Antibiotics are not routine. Your vet considers them when there’s evidence of bacterial lower-airway involvement (fever, lethargy, anorexia, productive/wet cough, crackles on auscultation, abnormal chest radiographs) or in high-risk patients (very young, geriatric, brachycephalic, or immunocompromised). Worsening cases may need nebulization, coupage, or IV fluids/oxygen if pneumonia develops. Dogs with canine influenza or complicated CIRDC are managed more aggressively and isolated.
Home care & recovery timeline
- Isolate from other dogs until your vet clears you (usually 10–14 days after cough onset or 5–7 days after cough stops, policy varies).
- Keep air smoke- and dust-free; avoid scented cleaners.
- Offer small, frequent meals and fresh water; use a slow, calm routine to limit cough spasms.
- Track a simple daily log: cough frequency, energy, appetite, temperature (rectal). If you see fever, listlessness, or rapid breathing, call your vet the same day.
Prevention that works (layer your defenses)
- Vaccinate per your vet’s guidance (Bordetella ± CPiV/CAV-2; influenza where indicated). Vaccines reduce severity and shedding, not all infections.
- Reduce exposure during known outbreaks; choose well-ventilated daycares and require proof of vaccines.
- For dogs with recurrent bouts, consider spacing high-risk activities and strengthening baseline parasite control and nutrition.
Red flags—go to the vet/ER now
- Breathing effort (abdomen heaving, flared nostrils), blue/grey gums, persistent fever, not eating >24 hours, collapse, bloody sputum, or a cough that worsens after 48–72 hours of rest/meds.
- Puppies, senior, brachycephalics, and dogs with heart/lung disease warrant earlier rechecks.
Bottom line: For kennel cough/CIRDC, the standard, most common treatment is supportive care with judicious use of vet-prescribed antitussives. Antibiotics are reserved for complicated or high-risk cases. Protect the community with isolation and vaccination, and escalate promptly if breathing changes or systemic signs appear.
(*) How To Handle All Dog Fleas
(**) How to Make Dog Food: Updated Guide & Expert Tips (2026)
(***) Top 10 Best Dog Carrier Backpack Hiking Reviews (Updated Guide)
3) Leptospirosis: Start Doxycycline Fast + Fluids

How it presents & how vets confirm it
Lepto often masquerades as “flu”—fever, lethargy, vomiting, diarrhea, muscle pain—then tips into kidney ± liver injury (PU/PD, jaundice). Because dogs shed leptospires in urine (it’s zoonotic), your vet treats it as contagious from the outset. Diagnosis is based on exposure history, exam and bloodwork (azotemia, liver enzyme changes), and specific tests: PCR on blood/urine in early illness, and MAT titers (paired or rising) to confirm. Catching it early matters because targeted antibiotics clear renal shedding and cut household risk. (See the 2023 ACVIM update for testing/treatment algorithms.)
The most common treatment (hospital-first)
Two pillars: antibiotics + supportive care. Current consensus favors doxycycline to eliminate organisms and stop urinary shedding—5 mg/kg PO q12h for 14 days is specifically recommended by the 2023 ACVIM statement. In very acute or vomiting dogs, clinicians often begin with an ampicillin/penicillin IV phase, then transition to doxycycline once the patient can keep oral meds down. Parallel care includes IV fluids, anti-nausea therapy, gastroprotectants, and close monitoring of kidney and liver values; dialysis can be life-saving in severe renal failure.
Post-exposure prophylaxis: For dogs with a credible exposure but no signs yet, many vets prescribe doxycycline for 14 days to prevent infection and renal carriage. Merck Veterinary Manual
Home care & zoonosis: protect your household
Finish every dose of antibiotics and follow your vet’s recheck plan (renal/liver panels, urinalysis). Handle urine as infectious: walk your dog in low-traffic areas, wear gloves to clean accidents, and disinfect surfaces. The CDC advises either an antibacterial cleaner or household bleach at 1:10 (one part bleach to ten parts water) for contaminated areas—apply, allow contact time, then rinse. Wash hands after removing gloves and launder soiled items hot. Keep other pets and people—especially kids, elders, and immunocompromised—away from urine until your vet confirms the dog is no longer shedding.
Vaccination & prevention (what actually lowers risk)
Lepto vaccination is risk-based but widely advised where the disease occurs. The AAHA 2022 canine vaccination guideline classifies leptospirosis as non-core, given according to regional risk and lifestyle; initial immunization is two doses 2–4 weeks apart, then annual boosters. The WSAVA 2024 global update goes further, recommending that in regions where lepto is endemic, the vaccine be treated as core for most dogs. Use multiserovar bacterins relevant to your area, control rodents/standing water, and avoid wildlife-contaminated puddles and streams.
Red flags—escalate now
Persistent vomiting, refusal to eat, increasing thirst/urination, yellow gums/eyes, blood in urine, or signs of dehydration warrant same-day veterinary care. Because lepto can worsen quickly and threatens people too, err on the side of calling your vet early.
4) Heartworm Disease: Doxycycline → Melarsomine (3-Dose) + Strict Rest

How it presents & how vets stage it
Heartworm can look sneaky at first—cough, exercise intolerance, weight loss, or just “slowing down.” Vets confirm infection with a heartworm antigen test (dogs ≥7 months) and often check for microfilariae (circulating larvae). Staging typically includes chest X-rays, CBC/chemistry, and urinalysis to gauge lung and heart strain and to classify disease severity (mild → severe/caval syndrome). Staging guides the safest treatment pace.
The most common treatment protocol (in plain English)
This is one of the clearest examples in the Most Common Treatment For 8 Diseases In Dogs playbook where sequence matters:
- Start immediately (Day 0–1)
- Begin a monthly heartworm preventive (macrocyclic lactone) to stop new larvae from maturing.
- Doxycycline for ~4 weeks (commonly 10 mg/kg/day split BID) to weaken Wolbachia—bacteria that live inside heartworms—and reduce lung inflammation when worms die.
- Strict exercise restriction begins now (crate rest/leash walks only). Activity drives complications.
- Cool-down period (Weeks 4–8)
- Finish doxycycline.
- Keep the preventive monthly.
- Many vets add short courses of anti-inflammatories if cough or inflammation is significant (only under veterinary direction).
- No running, no fetch, no daycare.
- Adulticide phase with melarsomine (the worm-killer)
- Injection #1 (Day ~60): one deep intramuscular shot into lumbar muscles.
- Strict rest continues; mild soreness is common—your clinic will give pain-control guidance.
- Injections #2 and #3 (Days ~90 & 91): two shots 24 hours apart. This 3-dose plan kills more adult worms more safely than a 2-dose plan, especially in moderate to severe disease.
- The danger window (first 4–8 weeks after final injection)
- As dead worms break up, pieces can embolize to the lungs. That’s why absolute activity restriction is non-negotiable after melarsomine—quiet crate life, short leash potty breaks.
- Rechecks & “test of cure”
- A microfilaria check is often done a few weeks after adulticide to confirm clearance.
- Antigen retest is typically done ~6 months after the last injection. Some dogs need additional work-up if the test stays positive.
Home care: what to do (and what to avoid)
- Enforce calm: think “bed rest” for a month after the last melarsomine shot. Elevated breathing rate, hard panting at rest, or coughing fits? Call your vet.
- Give meds exactly on schedule (preventive, any prescribed anti-inflammatories, cough control).
- Use a harness, not a neck collar, for gentle, controlled walks.
- Weight control: keep calories tidy—extra weight stresses the cardiopulmonary system.
- Do not try “slow-kill” (preventive-only) as a substitute for melarsomine unless your veterinarian has a specific medical reason; it prolongs disease, increases lung damage risk, and may contribute to resistance.
Complications & emergencies
Seek urgent care for labored or fast breathing at rest, collapse, pale/blue gums, severe lethargy, or dark/reddish urine. Dogs with caval syndrome (worms obstructing blood flow) require emergency surgical extraction before adulticide.
Prevention going forward
- Keep a year-round heartworm preventive on a set reminder.
- Combine with mosquito control (screens, avoid peak mosquito hours, repellents approved by your vet).
- Annual testing stays important—even on preventives—because missed doses or vomiting/spit-out pills happen.
Timeline snapshot you can screenshot
- Day 0: Positive antigen test → start preventive + doxycycline; strict rest begins.
- Day 1–28: Finish doxycycline.
- Day ~60: Melarsomine #1 → rest.
- Day ~90 & 91: Melarsomine #2 & #3 → the highest-risk embolism window follows; crate-level quiet for 4–8 weeks.
- Month 6 post-treatment: Antigen retest; discuss next steps if still positive.
Bottom line: For heartworm, the standard, safest course is doxycycline + monthly preventive followed by melarsomine in a 3-dose series, wrapped in strict exercise restriction from Day 0 until your vet clears activity. Prevention afterward is easier—and far safer—than treatment.
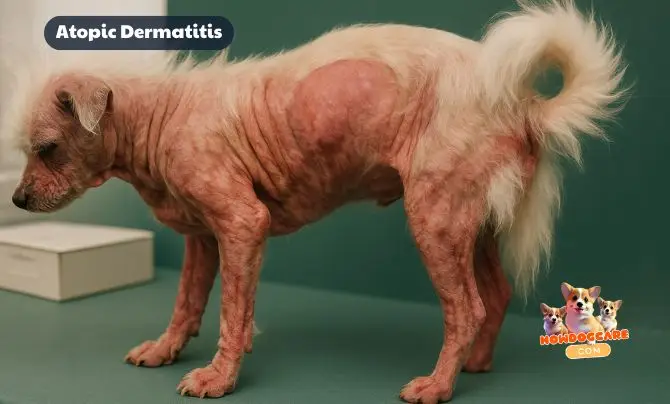
5) Atopic Dermatitis (Environmental Allergies): Multimodal, Not One-and-Done
What it looks like & what your vet rules out first
Relentless itching (paws, face, belly, ears), recurrent ear infections, and seasonal flares point to atopic dermatitis—an over-reaction to environmental allergens (dust mites, pollens, molds). Before calling it “atopy,” vets exclude parasites (fleas/mites), secondary infections (yeast/bacteria), and food allergy with an elimination diet when history suggests it. This stepwise approach is the current standard and prevents months of chasing the wrong trigger.
The most common treatment plan: layer fast relief + skin care + long-term control
Think toolbox, not a single pill. The evidence-based mix usually includes:
- Rapid itch relief (to break the scratch cycle)
- Oclacitinib (Apoquel)—oral JAK inhibitor; fast onset for pruritus control. Multiple randomized studies show significant itch and lesion reduction vs. placebo and parity with short steroid courses.
- Lokivetmab (Cytopoint)—injectable monoclonal antibody against IL-31; typically provides ~4–8 weeks relief; long-term safety/efficacy reports are favorable. Choice often hinges on patient factors and owner preference.
- Short steroid bursts can quell severe flares, but guidelines caution against routine long-acting injectables; use the lowest effective dose, shortest duration.
- Skin-barrier & infection control
- Weekly/biweekly medicated baths (antiseptic/antifungal shampoos), rinses/wipes, and ear therapies guided by cytology if otitis is present. Regular bathing reduces allergen load and helps many dogs need less drug over time.
- Treat any pyoderma/yeast promptly; recheck cytology to confirm resolution.
- Parasite control is mandatory
- Year-round flea prevention (isoxazolines preferred in AAHA guidance for combined flea/tick/mite cover and bath-tolerance). Even minimal flea exposure can supercharge itch (FAD).
- Long-game disease modification
- Allergen-Specific Immunotherapy (ASIT) (“allergy shots” or sublingual): the only treatment that can change the immune response. Meta-analyses/field data show ~60% of dogs improve ≥50% with good compliance and periodic rechecks. Best considered once environmental triggers are identified.
- Cyclosporine is a proven chronic controller when biologics or JAK inhibition aren’t ideal; onset is slower than oclacitinib/lokivetmab but well-supported in guidelines.
- Food trial when history hints at diet involvement
- A strict 6–8+ week elimination diet with a hydrolyzed or novel-protein food is the diagnostic gold standard for adverse food reactions; re-challenge confirms. Many “mixed” dogs have both atopy and food components.
What you do at home (consistency wins)
- Keep a flare diary (itch score 0–10, paws/ears/face, weather/pollen notes).
- Bathe/rinse on schedule; paw wipe-downs after walks help.
- Flea control every month without gaps.
- Follow the diet trial rules exactly (no off-diet treats/chews).
- Book planned rechecks—derm cases need tweaks, not “set and forget.” AAHA’s 2023 guideline emphasizes parasite control, topical therapy, and individualized anti-itch choices as the bedrock of care.
When to escalate or add tests
- Poor control despite appropriate meds and topicals.
- Frequent ear/skin infections or year-round signs → consider intradermal or serum testing to build ASIT.
- Suspicion of food allergy → do a formal elimination diet.
Bottom line
For atopic dermatitis, the Most Common Treatment For 8 Diseases In Dogs approach is multimodal: fast pruritus control (oclacitinib or lokivetmab), disciplined skin care and parasite prevention, plus ASIT for durable control—and a true diet trial when indicated. Layering these, per current guidelines, yields the best comfort with the least medication over time.
➡️ PetSafe Drinkwell Carbon Replacement Filters Review
👉 Top 10 Best Scented Dog Poop Bags Reviews
🏆 Top 10 Best Nebulizer Machines for Dogs Reviews
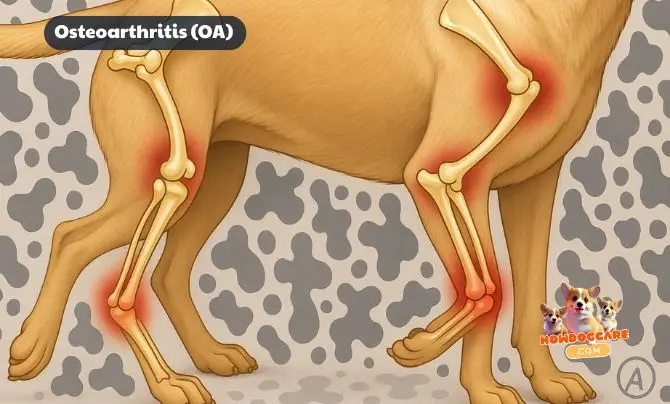
6) Osteoarthritis (OA): Combine NSAIDs, Weight Loss, Rehab & Omega-3s
What OA looks like & why a bundle works
Canine OA is a progressive, painful joint disease—stiffness after rest, reluctance to jump, slower walks, muscle loss, and “good days/bad days.” The Most Common Treatment For 8 Diseases In Dogs approach to OA isn’t one drug; it’s a multimodal bundle tailored to stage and comorbidities. Recent consensus (COASTeR) and international pain guidelines emphasize tiered care: analgesics + lifestyle + rehab + nutrition, adjusted over time.
1) NSAIDs = first-line pain relief
Veterinary NSAIDs (e.g., carprofen, meloxicam, deracoxib, firocoxib, grapiprant) remain the foundation when safe to use—reducing pain and inflammation so dogs can move, rebuild strength, and participate in rehab. Modern pain guidelines (AAHA/WSAVA) endorse using the lowest effective dose with periodic monitoring (exam ± labs) and layering other modalities rather than maxing any single drug.
2) Weight loss is medicine
For over-weight dogs, weight reduction alone can measurably improve lameness and force-plate metrics; several studies show meaningful gains once ~6–10% body weight is lost (more is better up to ideal BCS). Build a slow plan (≈0.5–1% BW/week) and reweigh every 2–4 weeks.
3) Rehabilitation & movement (what to actually do)
Combine controlled leash walks, cavaletti/step-over work, sit-to-stand reps, surface traction (runners, toe grips), ramps, and hydrotherapy as tolerated. Rehab plus analgesia improves mobility and quality of life; use validated owner tools (e.g., CBPI) to track progress and adjust.
4) Nutrition & omega-3s (EPA/DHA)
Dietary fish-oil omega-3s (EPA/DHA) reduce OA signs and improve weight-bearing in randomized trials; many dogs on omega-3–enriched diets also need less NSAID over time. Work with your vet on dose (commonly targeting combined EPA+DHA per kg BW/day) and choose products with quality testing.
Optional adjuncts: selected nutraceuticals (e.g., green-lipped mussel) show benefit in some studies, but products vary—use those with published data and third-party testing.
5) Anti-NGF monoclonal antibody (monthly injection)
Librela® (bedinvetmab), a monthly anti-nerve growth factor (NGF) monoclonal antibody, was FDA-approved in 2023 for canine OA pain and is widely used as part of multimodal care, especially when NSAIDs are insufficient or contraindicated. In late 2024, FDA issued a Dear Veterinarian letter summarizing post-approval adverse event reports (e.g., neurologic or urinary signs) and Zoetis updated U.S. labeling in 2025; decisions should weigh benefits vs. risks for each patient, with owners counseled and monitoring in place.
6) Sensible add-ons & when to escalate
- Adjunct analgesics (e.g., gabapentin, amantadine) for central sensitization or neuropathic components—layered under guideline oversight.
- Intra-articular options/biologics (case-by-case; evidence mixed) managed by orthopedics/rehab teams.
- Surgery (TPLO, total hip, etc.) when structural disease drives pain beyond medical control—your vet will stage and refer.
Your at-home game plan (checklist)
- Daily: short, frequent walks; traction mats; raised bowls; soft bedding.
- Weekly: weigh snacks, log mobility on a 0–10 scale, do home exercises, baths if recommended.
- Monthly: reweigh, review meds/supplements, and tweak calories.
- Every 3–6 months: veterinary recheck to reassess pain, function, labs (if on NSAIDs), and adjust the bundle. Consistency beats intensity in OA care.
Bottom line: In the Most Common Treatment For 8 Diseases In Dogs framework, OA care works best as a bundle—NSAID first-line, weight loss, rehab/mobility aids, and omega-3s, with anti-NGF mAb or other add-ons as needed and regular rechecks to keep comfort high and drugs low.
7) Otitis Externa (Ear Infections): Clean + Cytology-Guided Combo Drops

What it looks like & how vets confirm it
Head shaking, ear scratching, odor, discharge, and pain point to otitis externa. Your vet will examine the canal/ear drum and perform ear cytology (a quick swab stained and read under the microscope). Cytology distinguishes cocci (often Staph), yeast (Malassezia), or rods (often Pseudomonas) and drives treatment choices; it’s the cornerstone of evidence-based care. If the eardrum can’t be visualized, clinicians assume caution and tailor therapy accordingly.
The most common treatment plan (what works for most cases)
For uncomplicated otitis externa, the Most Common Treatment For 8 Diseases In Dogs playbook is:
- Thorough ear cleaning (in-clinic first, then at home),
- Topical “combo” drops that match cytology—typically antibiotic + antifungal + corticosteroid to address bacteria/yeast and inflammation,
- Recheck cytology to confirm resolution.
This approach resolves a large majority of cases when owners follow the plan and finish the full course.
Ear cleaning: products & technique
Proper cleaning improves drug contact and outcomes. Vets select cleaners based on the organism and debris: ceruminolytics for wax, antiseptic/acidifying agents for infected ears, and EDTA-based solutions (helpful against Pseudomonas) when rods are present. At home, massage cleaner into the canal, let it loosen debris, then wipe out with cotton balls or gauze—never cotton swabs down the canal. Frequency ranges from daily to weekly depending on discharge and vet guidance.
Picking the drop: match it to cytology
- Cocci/yeast: standard combo drops (antibiotic + antifungal + steroid).
- Rods/Pseudomonas suspected: culture is often advised; cleaners with EDTA and targeted topicals/systemics may be needed.
- Eardrum status uncertain/ruptured: avoid ototoxic agents; your vet will choose safer options.
Clinic-applied, long-acting gels such as florfenicol/terbinafine/mometasone (Claro in some markets) or florfenicol/terbinafine/betamethasone (Osurnia) can simplify compliance with one application that lasts weeks—used when appropriate and after exam.
When to culture or add systemic meds
You usually don’t need culture for a first, mild episode. Culture and susceptibility are recommended when you see rods on cytology, recurrent/chronic disease, treatment failure, suspected otitis media, or when systemic therapy is being considered. Systemic antibiotics are otherwise discouraged for simple otitis externa because topical therapy achieves higher local concentrations with fewer adverse effects.
Rechecks, timelines & underlying causes
Expect rechecks every 1–2 weeks until cytology is clear; many infections resolve in 2–4 weeks, but chronic cases can take longer. Address underlying problems—allergies (common), foreign bodies, anatomy (stenosis), swimming habits, or endocrine disease—to prevent relapse. Consistent follow-through is what converts “it keeps coming back” into “we’ve got this under control.”
Red flags—see your vet/ER
Severe pain, head tilt, facial nerve paresis, balance issues, or jaw pain may signal otitis media/interna and need advanced care (imaging, myringotomy, systemic therapy).
Bottom line: The standard, most common treatment for canine otitis externa is cleaning + cytology-guided topical combo drops, with culture/systemics reserved for rods, recurrence, or deeper disease—and rechecks to ensure you’re truly cured, not just “looking better.”
8) Diabetes Mellitus: Insulin + Diet Consistency + Monitoring

How it presents & how vets confirm it
Classic signs are excessive thirst/urination, weight loss despite good appetite, and sometimes recurrent infections. Vets diagnose with persistent hyperglycemia, glucosuria, and often elevated fructosamine; staging rules out complications (e.g., pancreatitis, DKA).
The most common treatment plan (what works for most dogs)
The backbone of care in any guide to the Most Common Treatment For 8 Diseases In Dogs is insulin therapy, started promptly and titrated carefully. First-line insulins for dogs are typically intermediate-acting preparations (e.g., lente/Vetsulin®, NPH) given twice daily, paired with a consistent feeding schedule. Your vet individualizes the starting dose, then adjusts to control clinical signs while avoiding hypoglycemia—the prime goal across all protocols.
Diet & feeding routine (make it boring—in a good way)
Pick a highly palatable, complete diet and feed the same amount at the same times every day so insulin timing matches nutrient absorption. Many dogs benefit from moderate dietary fiber, which can blunt post-meal glucose swings; fat restriction is considered when there’s hypertriglyceridemia or pancreatitis risk. Whatever food you choose, consistency beats brand.
Monitoring: curves, fructosamine & CGM (how dose changes really happen)
- Clinical signs first: thirst, urination, appetite, weight, energy.
- Blood glucose curves (BGCs): done at home or in-clinic to find the nadir and ensure safety; if BG dips too low, reduce the dose and re-curve.
- Fructosamine: reflects 2–3 weeks of control; interpret alongside clinical signs/BG data (single values don’t tell the whole story).
- Continuous glucose monitoring (CGM): devices like FreeStyle Libre provide near-real-time trends, catch nocturnal dips, and can simplify adjustments for many families.
At-home checklist (daily rhythm)
- Insulin at the same times every 12 hours; no doses if the dog won’t eat—call your vet.
- Meals right before/with insulin; no big between-meal snacks.
- Logbook: water intake, appetite, behavior, body weight weekly.
- Hypoglycemia plan: know signs (weakness, tremors, disorientation); offer food or rub Karo® syrup on gums and call the vet.
- Rechecks per your vet (curves, fructosamine), especially after any dose/diet change. Guidance from AAHA centers on controlling signs while avoiding lows.
When to escalate (don’t wait)
Go same-day if you see vomiting, diarrhea, lethargy, fruity breath, rapid breathing, collapse, or refusal to eat—possible DKA or severe hypoglycemia. Early intervention saves lives.
Long-term outlook & prevention notes
With engaged owners, most diabetic dogs live good, active lives. Keep body weight ideal, maintain a boring, repeatable routine, and use yearly screening in at-risk breeds or senior dogs to catch disease earlier—key themes echoed in AAHA guidance and standard references.
Bottom line: For diabetes, the standard, most common treatment is twice-daily insulin paired with dietary consistency and structured monitoring (curves, fructosamine, or CGM). Tight routines and proactive rechecks are what transform chaos at diagnosis into steady control at home.
(a) Human-Grade Dog Food (2026): Benefits, Costs & Top 10 Brands
(b) Top 10 Best Dog Muzzles Reviews (Updated Guide & Expert Tips)
(c) Best Dog Strollers 2026 | Top 10 Reviews, & Expert Buying Guide
(d) Top 10 Best Automatic Dog Waterer Outdoor Reviews
(e) Top 10 Best Outdoor Dog Kennel Reviews (Updated Guide & Tips)
(f) Top 10 Best Indoor Dog Gates Reviews (Updated Guide & Tips)
When First Aid Is Enough—And When It’s Not
Use this quick triage to decide what you can stabilize at home vs. what needs a vet now. It complements the care plans in The Most Common Treatment For 8 Diseases In Dogs and helps you act fast and appropriately.
First aid at home (then call your vet for guidance)
- Minor cuts/scrapes that stop bleeding with 5–10 minutes of steady pressure: clip fur, flush with saline, apply non-stick pad + wrap; schedule a same-day vet call for cleaning/antibiotics advice.
- Mild allergic hives without breathing trouble: keep dog calm, note timing/trigger, call your vet for antihistamine dosing (don’t DIY human meds).
- Simple split nail with controlled bleeding: pressure, styptic, light bandage; arrange a visit for trimming/pain control.
- Mild kennel cough signs (bright, eating, afebrile): rest, harness (no neck collar), humidified air; call your vet if cough persists >48–72 h. (Escalation signs below.)
Call your vet (same day)
- Repeated vomiting/diarrhea, especially puppies/seniors; any blood in stool or vomit.
- Limping or suspected sprain without obvious fracture.
- Ear discomfort (head shake/odor) but otherwise stable.
Persistent GI signs can dehydrate pets quickly—your vet will decide if outpatient care vs. ER is safest.
Go to the ER now (do not wait)
- Trouble breathing, nonstop coughing/gagging, blue/grey gums.
- Uncontrolled bleeding or bleeding >5 minutes despite pressure; deep/gaping wounds; eye injuries.
- Seizure >3 minutes, clusters, or first-ever seizure; collapse, suspected bloat/GDV (non-productive retching, distended belly), hit-by-car, snake bite, heatstroke, inability to urinate/defecate, or known/suspected poisoning.
Poisoning: who to call and what not to do
- Call ASPCA Animal Poison Control: (888) 426-4435 or Pet Poison Helpline: (855) 764-7661 for real-time instructions (fees may apply). These services tell you if and how to induce vomiting and what to do next. Do not induce vomiting unless a veterinarian or poison expert instructs you—it can be dangerous for many toxins and situations.
- In human exposures or if you’re unsure, U.S. Poison Control is also 24/7 at 1-800-222-1222.
Heatstroke first steps (while en route)
Move to shade/AC, start room-temperature water on body (not ice), use a fan, and head for the ER immediately. Avoid ice baths; over-cooling worsens outcomes.
Choking & seizures (safety rules)
If choking but still breathing, keep calm and go to the vet; only remove a visible object you can grasp without pushing it deeper. During seizures, don’t restrain, clear nearby objects, time the event, and seek care if it’s prolonged or recurrent.
Prep now (so you’re ready later)
- Keep a dog first-aid kit and an ICE card with clinic + ER addresses.
- Install the American Red Cross Pet First Aid app (step-by-steps, hospital locator).
Bottom line: First aid stabilizes; it doesn’t replace veterinary care. If breathing changes, bleeding won’t stop, neurologic signs appear, or you suspect toxins, choose the ER. When you’re unsure, call your vet or a poison hotline—faster decisions save lives.
Conclusion
If you remember nothing else from this guide, remember the pattern: act early, follow the evidence, and be consistent at home. The Most Common Treatment For 8 Diseases In Dogs isn’t eight mysterious formulas—it’s a clear playbook you can recognize and support.
- Acute infections: Parvo survives with hospital-level supportive care; kennel cough is mostly supportive unless complicated; leptospirosis needs doxycycline + fluids fast (and strict hygiene); heartworm follows doxycycline → melarsomine (3-dose) + strict rest.
- Chronic conditions: Atopic dermatitis improves with a multimodal plan (rapid itch control, skin care, parasite prevention, and often immunotherapy). Osteoarthritis responds best to a bundle (NSAIDs, weight loss, rehab, omega-3s). Otitis externa clears fastest with cleaning + cytology-guided drops and rechecks. Diabetes stays stable with insulin, diet consistency, and structured monitoring.
Your role is powerful: keep vaccines and preventives current, maintain an ideal body weight, use a simple health log (appetite, thirst/urination, stool, cough, activity, weekly weight), and never skip rechecks—most adjustments are small but meaningful. Stock a canine first-aid kit and an ICE card, and review the “When First Aid Is Enough—And When It’s Not” section so you know when to head straight to the ER.
The real secret behind the Most Common Treatment For 8 Diseases In Dogs is partnership—evidence-based veterinary care plus a calm, prepared owner at home. Do that, and you’ll turn scary moments into manageable plans and give your dog the longest, happiest runway possible.
FAQs About the Most Common Treatment For 8 Diseases In Dogs
What does “the most common treatment for 8 diseases in dogs” actually mean?
It’s a practical shorthand for the standard, evidence-based care vets use most often for eight high-impact conditions: parvovirus, kennel cough (CIRDC), leptospirosis, heartworm disease, atopic dermatitis, osteoarthritis, otitis externa (ear infections), and diabetes. Your vet still tailors the plan to your dog’s age, severity, and other health issues.
Can parvovirus be treated at home with fluids and rest?
No. Parvo survival hinges on hospital care—IV fluids/electrolytes, anti-nausea meds, antibiotics for secondary infection risk, and early nutrition. Some clinics may add an anti-parvovirus monoclonal antibody as an adjunct. Home care comes after stabilization and discharge.
My dog has a hacking cough—do they always need antibiotics?
Not usually. For uncomplicated kennel cough/CIRDC, the most common treatment is supportive care (rest, humidified air, harness instead of collar, antitussives when appropriate). Antibiotics are reserved for complicated or pneumonic cases, or high-risk patients.
Leptospirosis scares me—what should I do first?
Call your vet immediately. Typical care is doxycycline (often after an initial penicillin-class phase) plus IV fluids. Because lepto is zoonotic, handle urine with gloves and disinfect surfaces; your vet will give hygiene instructions. Vaccination is advised where risk exists.
Why is exercise restriction so strict during heartworm treatment?
When adult worms die after melarsomine injections, fragments can lodge in the lungs. Strict rest—from the day treatment starts until your vet clears activity—reduces life-threatening complications. Expect a staged protocol: preventive + doxycycline → melarsomine (3-dose).
What’s the fastest itch relief for atopic dermatitis?
Vets commonly start oclacitinib (Apoquel) or lokivetmab (Cytopoint) for rapid relief, add topical therapy (medicated baths/wipes), and control fleas year-round. Long-term, consider allergen-specific immunotherapy (ASIT) to reduce future drug dependence.
Can joint supplements replace NSAIDs for osteoarthritis?
Supplements can help some dogs, but the first-line pain control is a veterinary NSAID (if your dog can safely take one), combined with weight loss, rehab/exercise plans, home modifications, and omega-3s. Newer options (e.g., monthly anti-NGF monoclonal antibody) can be layered in when needed.
Why do my dog’s ear infections keep coming back?
Most recurrences happen when the underlying cause (often allergies) isn’t controlled or the original infection wasn’t fully cleared. The standard approach is ear cytology-guided drops (antibiotic + antifungal + steroid), proper cleaning technique, and rechecks until the canal is truly clear.
My newly diabetic dog feels overwhelming. What’s the daily routine?
Twice-daily insulin on schedule, feed the same diet at the same times, and keep a simple log (water intake, appetite, energy, weekly weight). Your vet adjusts the dose using glucose curves, fructosamine, or CGM data—never change doses without guidance.
When are antibiotics appropriate for coughs or ears?
- Coughs: only when there’s evidence of bacterial lower-airway disease or complications.
- Ears: most cases respond to topical combo drops; systemic antibiotics are reserved for rods, severe/refractory infections, or middle-ear involvement—guided by cytology/culture.
Do diet changes help with diabetes or skin disease?
Yes—consistency is key in diabetes, sometimes with moderate fiber or fat adjustments (if pancreatitis/triglycerides are issues). For skin, a strict elimination diet (hydrolyzed or true novel protein) may diagnose food allergy that’s amplifying itch.
How quickly should I see improvement?
- Parvo/lepto: improvement is tied to early, aggressive treatment.
- Kennel cough: most uncomplicated cases improve in 7–10 days.
- Allergies: relief can be hours–days with modern anti-itch meds; ASIT takes months.
- OA: days to weeks for comfort; weight-loss benefits build over weeks–months.
- Diabetes: stabilization often needs several weeks of dose adjustments.
Is it safe to use human OTC meds for my dog?
Only with vet approval. Many human products (decongestants, some cough/cold meds, NSAIDs like ibuprofen/naproxen) are dangerous to dogs. Always ask before giving anything.
Which vaccines and preventives truly matter against these 8 diseases?
- Core vaccines (parvo combo) protect against parvovirus.
- Bordetella/CPiV/CAV-2 reduce kennel cough risk/severity.
- Leptospirosis is recommended where endemic.
- Year-round heartworm preventive is non-negotiable.
Your vet will tailor a schedule to your region and lifestyle.
How do I know when first aid is enough vs. when to go to the ER?
First aid is fine for minor wounds, simple split nails, or uncomplicated cough in a bright, afebrile dog—follow up with your vet. ER now for breathing difficulty, uncontrolled bleeding, seizures, suspected poisoning, heatstroke, eye injuries, collapse, or bloat signs (retching with distended belly).
What should I track at home to help my vet?
Keep a one-page log: temperature, respiratory rate at rest, appetite, thirst/urination, stool quality, cough frequency, lameness score, and any meds given (with times). Good notes speed up diagnosis and fine-tuning treatment across all eight conditions.
Can I prevent most of these problems?
You can reduce risk dramatically with vaccination, parasite preventives, ideal body weight, dental care, and fast vet visits when something’s off. Prevention plus early action is the real secret behind the Most Common Treatment For 8 Diseases In Dogs working as well as it does.






